Seborrheic Dermatitis on the Face and Scalp — How to Identify, Manage, and Prevent Flare-Ups
Seborrheic dermatitis often shows up in the most visible areas of the body: the scalp, eyebrows, sides of the nose, eyelids, and behind the ears. Because of this, it can be both physically uncomfortable and socially frustrating. Understanding how it behaves specifically on the face and scalp is key to managing it effectively.
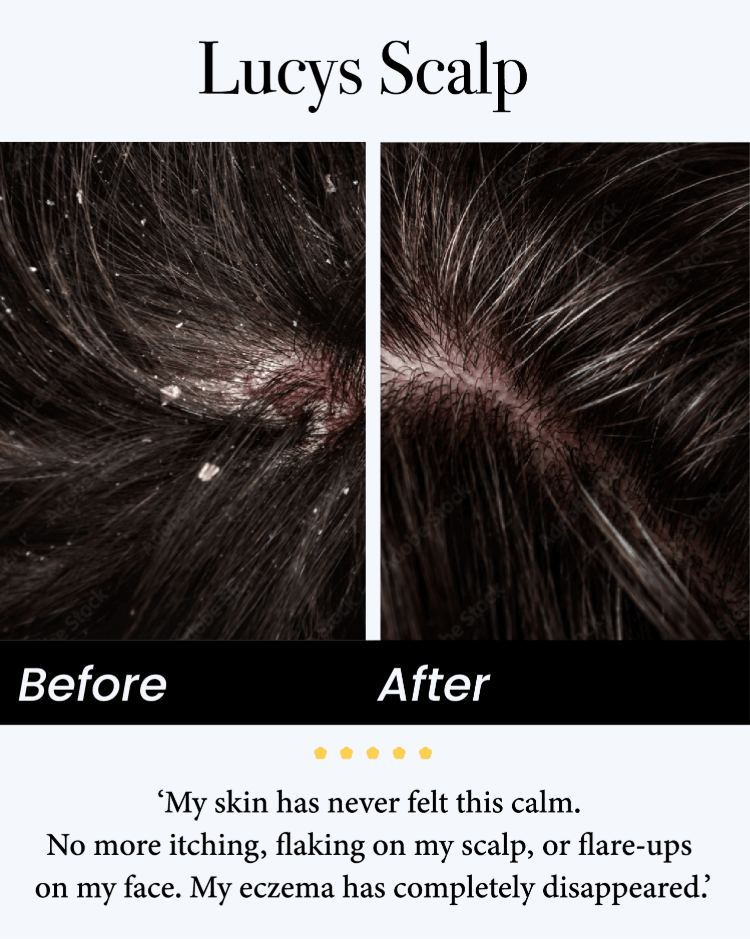
What it looks like on the scalp
On the scalp, seborrheic dermatitis is commonly mistaken for dandruff. However, it is usually more persistent and inflammatory than simple flaking.
Typical signs include:
-White or yellowish flakes
-Greasy or oily patches of skin
-Itching that can range from mild to intense
-Redness along the hairline or crown
-Flaking that falls onto shoulders or becomes noticeable in hair
In more severe cases, the scalp can feel tender or irritated, especially after scratching or using harsh shampoos.
One of the most important things to understand is that scalp seborrheic dermatitis is not caused by dry skin. In fact, it often occurs in oily conditions, which is why using heavy oils or avoiding washing altogether can sometimes worsen symptoms.
Seborrheic dermatitis on the face
Facial involvement tends to affect areas where oil glands are more active. The most common regions include:
-Sides of the nose (nasolabial folds)
-Eyebrows
-Eyelids
-Forehead
-Beard area in men
-Around the ears
Symptoms on the face may appear as:
-Red or pink patches
-Greasy-looking skin
-Flaking or peeling skin
-Mild swelling or sensitivity
Because facial skin is more delicate than the scalp, it tends to react more quickly to both triggers and treatments.
Why these areas are affected
Seborrheic dermatitis targets sebaceous gland–rich regions because these areas produce more sebum (skin oil). This oil provides an environment where a naturally occurring yeast called Malassezia can thrive.
In susceptible individuals, the immune system reacts to this yeast, triggering inflammation. The result is an overproduction of skin cells, leading to visible flaking and irritation.
This explains why the condition often appears in a “map-like” pattern across the face and scalp rather than randomly across the body.
Common triggers for facial and scalp flare-ups
While the underlying cause remains the same, flare-ups are often influenced by external and internal triggers:
1. Weather changes
Cold, dry air in winter is a major trigger, while humidity can also contribute for some people.
2. Stress
Emotional stress is strongly linked to worsening symptoms, likely due to immune system activation.
3. Skincare and haircare products
Harsh cleansers, alcohol-based toners, and heavily fragranced products can irritate the skin barrier.
4. Overwashing or underwashing
Both extremes can worsen symptoms. Overwashing strips the skin barrier, while underwashing can increase oil buildup.
5. Hormonal fluctuations
Changes in hormone levels can affect oil production, indirectly influencing flare-ups.
Effective management strategies
Managing seborrheic dermatitis on the face and scalp requires a combination of antifungal treatment, gentle care, and consistency.
Scalp care
Medicated shampoos are the backbone of scalp treatment. Ingredients that are commonly used include:
-Ketoconazole
-Zinc pyrithione
-Selenium sulfide
These shampoos work best when left on the scalp for several minutes before rinsing. Most people benefit from using them a few times per week rather than daily.
Between treatments, a mild, non-medicated shampoo can help maintain balance without over-stripping oils.
Facial care
Facial treatment is more delicate and usually involves:
-Gentle, fragrance-free cleansers
-Antifungal creams prescribed or recommended by a pharmacist or dermatologist
-Light moisturisers that do not clog pores
-In some cases, non-steroidal anti-inflammatory creams
Avoiding aggressive exfoliation is important, as this can worsen irritation and prolong healing.
Prevention: keeping flare-ups under control
While seborrheic dermatitis cannot always be prevented, flare-ups can often be reduced in frequency and severity.
Helpful long-term strategies include:
-Maintaining a consistent skincare routine
-Using antifungal treatments at the first sign of symptoms
-Avoiding unnecessary product changes
-Managing stress levels
-Protecting skin from extreme weather conditions
Consistency is more effective than intensive short-term treatment cycles.
Living with visible symptoms
Because seborrheic dermatitis often affects visible areas like the face and scalp, it can impact confidence. However, it’s important to recognize that it is a common and manageable condition.
Most people experience cycles of improvement and flare-ups rather than constant symptoms. With the right routine, many are able to keep the condition mild and barely noticeable.
The goal is not perfect skin, but stable skin that you can reliably manage.