Is Eczema Genetic? What Family History Really Means
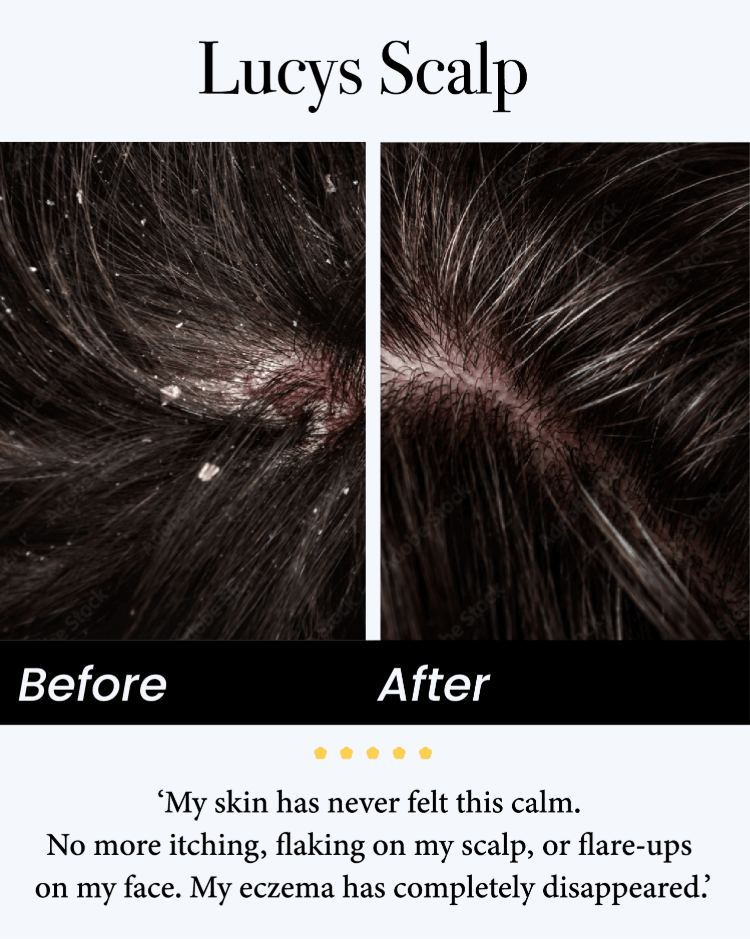
Eczema, also known as atopic dermatitis, is a chronic skin condition marked by red, itchy, and inflamed patches. It often develops in childhood but can persist or appear in adulthood. Many people wonder: “If my parents or siblings have eczema, will I get it too?” The answer isn’t as simple as a yes or no—it involves genetics, environment, and immune system factors.
Understanding Eczema
Eczema is an inflammatory skin disorder caused by a combination of immune system dysregulation, skin barrier defects, and environmental triggers. Symptoms can vary from mild dryness to severe itching and painful inflammation.
Key features include:
-Dry, sensitive skin
-Intense itching
-Red or brownish-gray patches
-Small, raised bumps that may ooze or crust
While eczema itself is not contagious, it can run in families, suggesting a genetic component.
The Genetic Component of Eczema
Research shows that eczema has a strong genetic basis, though it is not caused by a single gene. Instead, multiple genes can increase susceptibility.
Important Genetic Factors
-
Filaggrin Gene Mutations (FLG)
- Filaggrin is a protein essential for skin barrier integrity.
- Mutations in the FLG gene can weaken the skin’s barrier, making it more prone to dryness and irritation.
- Individuals with these mutations are at higher risk of developing eczema.
-
Immune System Genes
- Variations in genes regulating the immune system can cause heightened inflammatory responses to irritants or allergens.
-
Other Atopic Conditions
- Genes linked to asthma and allergic rhinitis often overlap with eczema, explaining the “atopic march” where one condition may lead to another.
Bottom line: Eczema is genetic, but inheritance is complex. Having a parent with eczema increases your risk, but it doesn’t guarantee you will develop it.
What Family History Really Means
Family history can provide clues about risk, but it doesn’t determine destiny.
-One parent with eczema → Your child has roughly a 20–30% chance of developing it.
-Both parents with eczema → The risk rises to about 50–60%.
-Family history of other atopic conditions → Even without eczema in parents, a child may still be predisposed if asthma or allergies run in the family.
Key takeaway: Genetics is only part of the story—environmental triggers, diet, skin care, and exposure to allergens all influence whether eczema manifests.
Environmental and Lifestyle Influences
Even if you have a genetic predisposition, certain factors can trigger or worsen eczema:
-Dry climate or low humidity – Can strip moisture from the skin.
-Irritants – Harsh soaps, detergents, and fragrances.
-Allergens – Pollen, pet dander, dust mites.
-Stress – Emotional stress can exacerbate inflammation.
-Infections – Bacterial or viral infections can worsen flare-ups.
Managing these factors can significantly reduce flare-ups, even for genetically predisposed individuals.
Prevention and Management Strategies
While you can’t change your genes, you can take proactive steps:
- Moisturise Daily – Thick creams or ointments help repair the skin barrier.
- Use Gentle Skincare Products – Avoid fragrances, harsh chemicals, and alcohol-based products.
- Identify Triggers – Keep a symptom diary to link flare-ups to foods, environmental factors, or stress.
- Follow Medical Advice – Topical corticosteroids, calcineurin inhibitors, or newer biologic treatments may be prescribed for moderate to severe cases.
- Consider Early Intervention for Children – Regular moisturizing and gentle care from infancy can reduce severity, even in high-risk children.
Bottom Line
Yes, eczema has a genetic component, but it is not purely inherited in a simple pattern. A family history of eczema or other atopic conditions increases your risk, but lifestyle, environment, and immune responses also play a crucial role. Understanding both the genetic and environmental sides of eczema empowers families to take preventive steps and manage symptoms effectively.
In short: Genetics loads the gun, but environment often pulls the trigger.